Hip replacement surgery (hip arthroplasty)
The damaged hip joint is replaced with a new, artificial one.
We offer advanced surgical techniques and expert aftercare to replace painful damaged hip joints and help you get back to everyday activities.
Sometimes also called
- Hip arthroplasty
At a glance
-
Typical hospital stay
2–5 days -
Procedure duration
60–90 minutes -
Type of anaesthetic
General, spinal or epidural -
Available to self-pay?
Yes -
Covered by health insurance?
Yes
Why Spire?
- Fast access to treatment when you need it
- Internationally and nationally renowned consultants
- Flexible payment options to help you spread the cost
- 98% of our patients are likely to recommend us to their family and friends
What is hip replacement surgery?
A hip replacement is a common operation to remove worn or damaged parts of your hip joint and replace them with an artificial joint to help you move more easily and to reduce pain. Conditions such as osteoarthritis or a hip fracture can make it hard to manage everyday tasks eg getting dressed, having a bath or walking. Chronic (long-term) pain can also prevent you from sleeping well and enjoying life.
Signs of needing a hip replacement
Hip pain is the main reason why you might need hip replacement surgery, particularly if:
- Non-surgical treatments haven’t relieved your hip pain
- You have hip pain even when you are not standing or walking
As well as hip pain, hip replacement surgery may benefit you if you have:
- Difficulty with daily activities, such as shopping or bathing
- Depression due to pain or lack of mobility
- Hip problems that affect your work or social life
- Hip swelling, stiffness and reduced mobility eg stiffness in your hip that prevents you from lifting up your leg
- Reduced quality of life or disturbed sleep
Most people who have hip replacement surgery are aged between 60 and 80. However, teenagers with juvenile arthritis may also have hip replacement surgery. Your doctor may recommend it if you have:
- A hip fracture
- Ankylosing spondylitis
- Osteoarthritis
- Rheumatoid arthritis
- Septic arthritis
- Unusual bone growth
When determining whether you are suitable for hip replacement surgery, your doctor will also consider risk factors for complications after surgery, such as your age, weight and whether you have diabetes.
If you are healthy and in good physical condition, the chances of any given complication are low, between 0-3%. However, if you have several risk factors, the chances of complications rise to around 20%.
Is hip replacement surgery right for you?
Hip replacement can ease pain and allow you to become more active again. However, it may not be suitable for you if the risks of surgery outweigh the benefits or you’re unable to cope with the recovery afterwards.
Before you decide to go ahead with hip replacement surgery, you should discuss the pros and cons with your doctor and research what’s involved before, during and after the operation.
As well as the potential benefits of reducing pain, increasing mobility and improving your quality of life, you should consider that:
- As with all major surgery, there are some risks of complications
- You may not be able to take part in certain sports or perform some movements, such as squatting
- You will be less mobile for the first few weeks after the operation so you may need some help around the house and with errands
- Your new hip joint may eventually need revision surgery after 10-20 years
Alternative treatments to hip replacement surgery
Your doctor will usually recommend hip replacement surgery only after you’ve tried other treatments that haven't worked for you.
Non-surgical treatments include:
- Pain or anti-inflammatory medication
- Physiotherapy — your physiotherapist might also recommend changes to specific movements you make to ease your symptoms
- Steroid injections
- Walking supports, such as a cane
- Weight loss
Hip resurfacing
This surgery involves removing the damaged surface of your hip bone and replacing it with a metal surface. It is usually used to treat men who have an active lifestyle and have larger hips. However, this surgery is less common today as there are concerns about damage to surrounding soft tissues.
Subchondroplasty
This procedure is used to promote natural bone growth. It involves injecting a bone substitute into your hip joint to fill any gaps. Over time, the bone substitute is absorbed by the body and replaced with natural bone.
Orthopaedic evaluation
Your doctor will perform a physical examination of your hip and ask about your medical history to assess your general health.
You will need an X-ray so your doctor can better assess your hip. You may also need a CT scan or MRI scan. You can use our fast diagnostic services so you won’t have to wait long to find out if hip replacement surgery is right for you. Your consultant will discuss what would be best for you and your lifestyle.
Find a Spire hospital offering hip arthroplasty
Almost all our hospitals offer private hip replacement surgery and have teams of orthopaedic (bone and muscle) surgeons who specialise in this procedure.

Events
Exclusive patient information event on knee pain treatments
Patient information event regarding knee pain treatment options not currently on the NHS, with special focus on Arthrosamid injections.
Learn more
Free patient event - hip arthritis: is hip replacement right for you?
Information event and free mini consultations with Mr Alun John, Consultant Orthopaedic Hip Surgeon at Spire Cardiff Hospital.
Learn more
How a hip replacement works
In a healthy hip joint
Your hips are ball-and-socket joints and are the biggest joints in your body. The ball part is the head of your thigh bone (femur), which sits in a socket made of a hollow in your pelvic bone called the acetabulum — these two bones are connected by ligaments, which stabilise the joint and form the hip capsule.
The surfaces of the bones in your hip joint are coated with smooth, slippery cartilage, which protects and cushions your bones, allowing them to move easily next to each other. This is surrounded by a thin tissue called the synovial membrane, which produces a fluid to lubricate your joint and its cartilage.
In an unhealthy hip joint
When the cartilage is worn or damaged, it makes your bones rub together. This can cause your hip to become stiff and can be very painful.
Types of hip replacement surgery
Hip replacement surgery can be performed either by making a cut into the side or back of your hip (posterior hip replacement) or the front (anterior hip replacement).
There are pros and cons to each of these approaches. Posterior hip replacement is more common and gives your surgeon a better view of your hip joint. Anterior hip replacement is less common and may have a higher risk of nerve damage — this can cause numbness in your outer thigh.
You will usually be admitted to hospital on the day of your surgery and will discuss your procedure with your surgeon. An experienced surgeon will perform your surgery, sometimes helped by more junior doctors — during your pre-operative assessment, you will be told who will perform your surgery.
Total hip replacement
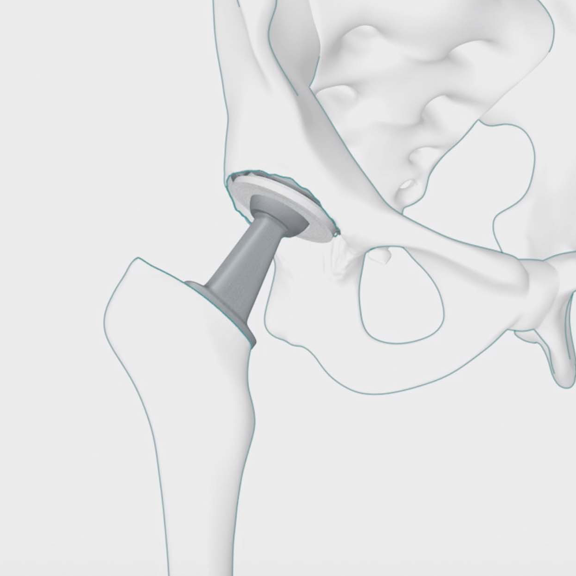
In a total hip replacement operation, your surgeon will hollow out your hip socket and remove the top of your thigh bone. To create your new joint, they’ll implant a new socket (cup) in the hollow of your pelvis and insert a rod (stem) with a ball at the upper end into your thigh bone. A spacer made of plastic, ceramic or metal will be placed between the ball and cup to create a smooth gliding surface.
The new components are fixed to your bones using acrylic cement. Although, if you’re more active, you can have one or both parts fixed without cement. In these cases, the implant surface is roughened or coated in a special material that helps encourage natural bone growth and fusion with the implanted prostheses.
Hip joint implants can be made from ceramic, metal or plastic. The most common combination of prostheses is a metal ball and plastic socket. Alternatively, and often used if you’re younger or more active, you can have a ceramic ball with a ceramic or plastic socket.
Your doctor will recommend the best option for you by considering:
- How active you are now and plan to be in the future
- The shape of your hip
- Your age
- Your natural hip size
It’s even possible to have implants tailor-made for an even better fit.
Minimally-invasive hip replacement surgery
Most hip replacement surgery is carried out using a large 20-30cm cut. However, a newer procedure called minimally-invasive hip replacement uses one or two smaller cuts, around 10cm in length, and special instruments to replace the joint. This procedure is safe and effective, and can reduce muscle damage, pain after surgery and recovery time.
Minimally-invasive hip replacement is usually offered if you are under 50, in good health and have a healthy body mass index (BMI).
Bilateral hip replacement
If you need both of your hips replaced, your surgeon may recommend replacing one hip first, allowing for a period of recovery, and then replacing the second hip. However, bilateral hip replacement involves replacing both hips at the same time. This surgery is longer and therefore means spending more time under general anaesthesia. It also has a greater risk of blood loss.
Hip joint implants
There are several different types of hip implants:
- Ceramic-on-Ceramic (CoC) — the ball is ceramic and the socket (cup) has a metal lining
- Ceramic-on-Polyethylene (CoP) — the ball is ceramic and the cup is plastic or has a plastic (polyethylene) lining
- Metal-on-Metal (MoM) — the ball and cup are metal; these are rarely used as they come with a greater risk of complications
- Metal-on-Polyethylene (MoP) — the ball is metal and the cup is plastic or has a plastic (polyethylene) lining
Your surgeon will discuss which type of hip implant is most appropriate for you.
Total hip arthroplasty
Watch how a hip replacement surgery takes place
View transcript of this video
This video explains what happens during a hip replacement surgery. A hip replacement is a common operation to remove worn or damaged parts of your hip joint and replace them with an artificial joint. It is often recommended if other treatments such as physiotherapy or steroid injections haven't helped reduce pain or improve mobility.
Your hip is the joint between the thigh bone or femur and the pelvis. The pelvis contains three bones called ilium, ischium, and pubis.
The hip joint is a ball-and-socket joint. The round head of the femur rests in a cavity, the acetabulum, that allows the rotation of the limb. The surface of these bones is coated with smooth, slippery cartilage also called articular cartilage which protects and cushions your bones allowing them to move easily next to each other.
When the cartilage is worn or damaged, the bones rub against each other causing pain and lack of mobility. Under an aesthetic, the surgeon will remove both the socket and the top of your thigh bone. The replacement components are the metal head and a plastic cup which are then inserted back into the socket of your pelvis.
A replacement ball on a stem will be inserted into your thigh bone. The ball is then placed into the socket putting your hip joint back together.
The surgery usually takes around 90 minutes. You should be able to leave the hospital after three to five days.
For the first weeks after the surgery, you'll need a walking aid such as crutches to help support you. Physiotherapy will help strengthen your muscles and ensure your new hip works at its best. For more information, contact your local Spire hospital or visit the Spire Healthcare website.
What to expect during hip replacement surgery
Preparing for hip replacement surgery
It’s important to stay as active as possible before the operation to strengthen the muscles around your hip and therefore improve your recovery. If you can continue with gentle exercise (eg walking, swimming) in the weeks or months running up to your surgery this will help.
You may be seen by a physiotherapist who can give you advice about particular exercises you can do to help before and after your operation.
Before your operation, you’ll need a pre-operative assessment with a nurse to ensure that you’re fit enough for surgery. Your nurse or consultant will tell you what this will involve and give you instructions on how to prepare in the days leading up to your operation.
It’s best to arrange for someone to take you home and help you around the house for the first few days after surgery. It’s also a good idea to prepare your home for after your operation to make it easier for you to get around safely and more easily — remove anything you can trip over and make sure important items are easy to reach.
Anaesthetic
Hip replacement surgery is usually done under general anaesthetic, where you’ll be unconscious during the operation. This usually means you won’t be able to eat anything for six hours or drink anything for two hours before your procedure. However, some patients may have an epidural anaesthetic, where you're awake but won’t be able to feel anything from the waist down. If you have this option, you may have a sedative to help you feel more relaxed. Your consultant will discuss with you what’s best in your case. On the day, you’ll be seen by an anaesthetist who will administer your anaesthetic before your operation.
How long does a hip replacement take?
Usually between 1 hour and 90 minutes.
Pain after hip replacement surgery
As with most operations, you’re likely to feel some discomfort afterwards, which may last a few days or weeks. You’ll be given painkillers and we can help you manage any pain as you recover. The good news is the chronic pain you felt before your hip replacement should go away, so you should be yourself again in a few months.
Your hospital stay
The average hospital stay is two to five days.
Hip replacement surgery recovery
How quickly you recover from your surgery depends on how fit you were before and on the type of operation you have.
When you wake up from surgery, you’ll probably have a pillow between your legs to keep your hip in the correct place. You’ll have some dressings on your wounds and stitches that will be removed by a nurse or doctor around a week or so after your operation, or they’ll disappear by themselves if they’re dissolvable.
In the short term, you may feel some of the side effects of general anaesthetic, which include nausea and vomiting. You may also be constipated, so try to drink plenty of fluids and eat high fibre foods. If this doesn’t help, your doctor can prescribe some medication.
To prevent deep vein thrombosis, you’ll need to wear compression stockings and try to get active again as soon as you can do so safely.
Your condition will be monitored during your recovery.
Physiotherapy and ongoing treatment
While you're in hospital, a physiotherapist will take you through a series of exercises to strengthen your muscles and to help your new hip work at its best. At home, it’s important to do these exercises after hip replacement surgery to speed up your recovery so you can start to enjoy everyday life again.
Physiotherapy and exercises after a hip replacement
If you have minimally-invasive hip replacement surgery, you may be able to walk on the same day as your operation.
Your physiotherapist will teach you how to sit, stand and bend in a way that avoids damaging your hip. They will put together a programme of activity to help your recovery, which will include:
- A graduated walking plan — this will slowly increase your mobility around the house and eventually outside
- Resuming normal activities around the house, such as climbing stairs, sitting and standing
- Targeted daily exercises — this will help restore your movement and strengthen your hip; in the first few weeks, you may need help from your physiotherapist at home or at a clinic to help you with these exercises but as you recover, you will be able to do them by yourself
Your lifestyle after treatment
You should expect to be pain-free and to move more easily, without any stiffness in your hip. Your consultant will discuss how to enjoy your usual activities safely. You may be advised to avoid some activities that risk over-extending or dislocating your new hip eg extreme sports.
Looking after your new hip
In the initial weeks after surgery, you should avoid applying pressure to your wound. You should therefore avoid lying on your side.
You should also avoid:
- Bending your hip more than 90 degrees
- Crossing your legs over each other
- Forcing your hip into uncomfortable positions
- Sitting on low chairs and toilet seats — you can have a raised toilet seat fitted at home
- Swivelling on the ball of your foot
- Twisting your hip
You should:
- See your orthopaedic surgeon for routine follow-up examinations and X-rays — you should do this even if your hip feels fine
- Take small steps when turning around
- Take part in regular, light exercise to maintain the strength and mobility of your new hip
- Tell your dentist that you have had a hip replacement — ask your orthopaedic surgeon whether you need to take antibiotics before having any dental procedures
- Use a walking aid and take other precautions to avoid falls
How long does a hip replacement last?
A modern artificial hip joint replacement should last for 15 years or more. Only 7 in 100 hip joint replacements need further surgery after 13 years, according to the National Joint Registry (NJR).
Hip replacement recovery timeline
Everyone is different and your recovery will depend on:
- How fit you were before surgery
- The condition of your joints and muscles
- The type of work or other activities you do
- Your age
However, in general after a total hip replacement, you will need support to walk for the first one or two days after surgery, as well as help from a physiotherapist. You can leave hospital after 3-5 days. In 1-2 weeks you will be able to walk more using a walking aid.
After 2-6 weeks, you can progress to doing more exercises, such as gentle swimming and static cycling. You can return to desk-based work after 6-8 weeks and will most likely not need a walking aid anymore. Following advice from your surgeon, you may be able to drive again. You can also have sex but should avoid positions that could dislocate your hip.
If you perform manual work, you will need to wait for around 12 weeks before you return to work. You should feel normal again and be able to perform all of your usual activities.

Day 1
Week 12
1-2 days
Walk with support and help from a physiotherapist
3-5 days
You’ll be able to leave hospital
1-2 weeks
Walking more each day using a walking aid
2-6 weeks
Gradually able to do more exercises such as gentle swimming and static cycling
6-8 weeks
Return to work if desk based, no longer require walking aid, be able to drive if advised by your surgeon, and be able to have sex, but avoid positions of potential dislocation
12 weeks
Return to work for manual labour jobs, you should feel normal again and be able to perform your usual activities
-
1-2 days
Walk with support and help from a physiotherapist
-
3-5 days
You’ll be able to leave hospital
-
1-2 weeks
Walking more each day using a walking aid
-
2-6 weeks
Gradually able to do more exercises such as gentle swimming and static cycling
-
6-8 weeks
Return to work if desk based, no longer require walking aid, be able to drive if advised by your surgeon, and be able to have sex, but avoid positions of potential dislocation
-
12 weeks
Return to work for manual labour jobs, you should feel normal again and be able to perform your usual activities
Risks and complications of hip replacement surgery
Nine in 10 people can expect their hip replacement to be functioning 10 years after surgery. Cases of failure needing revision surgery are around 1% per year for the first five years.
The risk of serious complications is low and most people have hip replacement surgery without complications, but all surgery carries risks. Your consultant will talk you through any potential risks before you go ahead. They can include:
- Dislocation
- Fracture
- Infection at the site of the wound or urine infection
- Injuries to blood vessels or nerves and bleeding under your skin
- Joint stiffening
- One leg longer than the other
Infections occur in one in every 100 operations. However, at Spire Healthcare, we take all precautions possible to reduce the risk of infection — this includes ultra-clean conditions and prescribing antibiotics. In some cases, infection may be treated by washing out the hip replacement. If your wound leaks fluid or your pain increases call 111 or your GP.
Joint loosening is another potential complication, which occurs in five in every 100 operations and usually 10-15 years later. This happens because the stem of the implant loosens in the hollow of the thigh bone or because the bone around the implant becomes thinner. If this occurs, you may need revision surgery to repair it.
Wear and tear of the new artificial joint can also occur, causing tiny particles to break off and be absorbed by surrounding tissue. This can result in the joint loosening and will need careful monitoring with X-rays and possibly further surgery to correct.
Signs of serious complications after hip replacement surgery
You should contact your doctor urgently if, after your hip replacement surgery, you have warning signs of:
- A deep vein thrombosis (DVT) — this is a blood clot in your leg; signs include hard, hot, red or painful areas in your leg
- A pulmonary embolism — this is a blood clot that travels to your lungs and is rare; signs include chest pains or breathlessness
- An infection — signs include:
- A persistent fever
- Chills
- Increasing hip pain when active and at rest
- Leaking of fluid from your hip wound
- Redness, tenderness, or swelling of your hip wound that is getting worse
To reduce your risk of developing blood clots, you will be given blood-thinning medication and compression stockings. You should also move your legs as soon as possible after your operation — check with your nurse or physiotherapist about what movements are appropriate.
Risks of general anaesthetic
Serious complications associated with general anaesthetic do occur, but they're extremely rare. For most people, the benefits in terms of controlled unconsciousness and removal of pain are much greater than the disadvantages. It’s estimated that serious complications result in approximately four deaths for every million anaesthetics given. The pre-operative assessment is carried out to limit the risk of any complications occurring.
At Spire Healthcare hospitals, your safety is our top priority. We have high standards of quality control, equipment and cleanliness and an ongoing system of review and training for our medical teams.
Frequently asked questions
How soon will I be up and about?
Your care team will try to get you out of bed and mobile as soon as possible. This may even be the same day as your operation. You’ll be able to walk with crutches and the support of your physiotherapist while in hospital. You’ll be able to go home when your care team are happy with your recovery and that you'll be able to move around safely at home.
How long will it be before I feel normal?
You should be able to get back to normal daily activities around six weeks after your operation. However, it’s important to remember that everyone recovers differently and it’ll depend on your age, fitness level before the operation, the condition of the hip and your normal activities that you do.
When can I drive again?
Many people are able to drive again after six to eight weeks, but check with your surgeon first. You should also check with your motor insurance company, as many won’t insure you for a number of weeks after an operation.
When can I go back to work?
Getting back to work after a hip operation depends on the type of job you have. For desk-based jobs you should be able to return after six to eight weeks, while for manual labour jobs it could be around 12 weeks.
When can I do housework?
You should be able to get back to most daily activities including light chores after six weeks, although you should avoid any heavy lifting or strenuous activity for around three months after your operation.
How will it affect my sex life?
There’s no set time when it’s safe to have sex. You should treat it like any other physical activity during your recovery and gradually build up to it and only if it feels comfortable. Make sure you follow your physiotherapists advice about what movements to avoid.
Will I have to go back to the hospital?
You’ll return to hospital a few weeks after your operation for a follow-up appointment to check your recovery progress.
Will I need another new hip?
Most hip replacements last for at least 15 years. This means if you’re younger, you may need another operation to replace the worn joint. A repeat operation is more complex, with an increased risk of complications, and isn’t suitable for everyone.
Are there any sports or activities I shouldn't do after my hip replacement?
Your consultant will discuss how to enjoy your usual activities safely. You may be advised to avoid some activities, eg extreme sports that risk over-extending or dislocating your new hip. Try not to put stress on your hip by avoiding sitting cross legged, sitting very low or rotating your hip.
How can I make my recovery easier?
You can help your recovery by making sure you’re as fit as you can be before surgery and strengthening the muscles around your hip. After surgery, make sure you continue your physiotherapists exercises at home to help you get the most from your new hip.
When can I fly after hip replacement surgery?
Speak to your consultant or GP before flying to find out what’s right for you. It’s important to note that your chance of deep vein thrombosis (DVT) increases if you fly after recent surgery.
Airlines have their own regulations about passengers flying after surgery, so make sure you check beforehand.
What are hip implants made from?
Hip implants can be made from metal, plastic or ceramic components. The most common combination is a metal ball and plastic socket. Alternatively, and often used if you’re younger or more active, you can have a ceramic ball with a ceramic or plastic socket.
When can I bend down after hip replacement?
You can usually bend down 12 weeks after having a hip replacement. However, you should avoid bending your hip more than 90 degrees.
How long after hip replacement can I tie my shoes?
You should be able to bend to tie your shoes after you have fully recovered from your hip replacement surgery, which usually takes around 12 weeks. However, even after you have recovered, you should try to avoid bending your hip more than 90 degrees.
The treatment described on this page may be adapted to meet your individual needs, so it's important to follow your healthcare professional's advice and raise any questions that you may have with them.
Get in touch
Sources
https://orthoinfo.aaos.org/en/treatment/total-hip-replacement/
https://www.mayoclinic.org/tests-procedures/hip-replacement/about/pac-20385042
https://www.drugwatch.com/hip-replacement/
https://www.nhs.uk/conditions/hip-replacement/
https://www.nhs.uk/conditions/hip-replacement/what-happens/
https://www.nhs.uk/conditions/hip-replacement/risks/
https://www.nhs.uk/conditions/hip-replacement/metal-implants/
https://www.nhs.uk/conditions/hip-replacement/recovery/
https://www.fda.gov/medical-devices/metal-metal-hip-implants/general-information-about-hip-implants