What is bursitis of the hip?
Hip bursitis affects the bursae in your hips. These are small, fluid-filled sacs that sit between the bones in your joints and the soft tissue that surrounds them. They help your joints move smoothly by acting as cushions that reduce friction.
Bursitis occurs when the linings of the bursae (membranes) become irritated and inflamed. This can cause extra fluid to build-up in the bursae, which makes them swell.
Your hip joint contains two main bursae: the iliopsoas bursa and the trochanteric bursa — inflammation of these bursae can cause hip bursitis pain.
Trochanteric bursitis
The greater trochanter is the bony part of your hip on the side of your body, where your thigh curves outwards. The bursa that sits over this part of your hip is called the trochanteric bursa and when it gets inflamed it causes trochanteric bursitis.
Hip bursitis pain caused by inflammation of the trochanteric bursa occurs in your outer hip.
Common causes of trochanteric bursitis include:
- Excessive pressure on your hip joint eg due to a misshapen or poorly positioned joint
- Hip injury
- Inflammation or tears in the gluteus medius tendon (a tendon in your buttocks)
- Overuse due to activities that strain your hip joint
Iliopsoas bursitis
The iliopsoas muscle runs from your lower spine, through your hip and down to your thigh bone. The iliopsoas bursa sits under this muscle on the inner (groin) side of your hip joint and when it gets inflamed it causes iliopsoas bursitis or iliopectineal bursitis.
Hip bursitis pain caused by inflammation of the iliopsoas bursa occurs in your groin area and the front of your hip.
Iliopsoas bursitis is less common than trochanteric bursitis — both are diagnosed and treated in a similar way.
Septic hip bursitis
This occurs when either of the bursae in your hip joint becomes infected. This is rare but serious and requires immediate medical attention.
Symptoms of hip bursitis
Hip bursitis symptoms include:
- Pain in your hip — in the early stages, pain may feel sharp and intense and later become dull and achy; if you have trochanteric bursitis pain will occur in your outer hip, while if you have iliopsoas bursitis pain will occur in your groin area and front of your hip
- Pain that starts when you exercise or perform repetitive activities eg climbing up or down the stairs, squatting or walking
- Pain when you extend your leg to the side outwards (hip abduction) or inwards (hip adduction) eg when getting out of bed or a car or stepping sideways
- Radiating pain — pain that spreads to your buttocks, groin, lower back, outer thigh and knee
- Tenderness in and around your hip
- Worsening pain at night or when sitting for long periods of time
Symptoms of septic hip bursitis
If you have septic bursitis you may have the usual symptoms of hip bursitis mentioned above as well as the following symptoms:
- Fatigue — extreme tiredness despite getting enough sleep
- Feeling generally unwell
- Fever
- Warm, red skin around your hip
Septic hip bursitis needs immediate medical treatment to stop the infection spreading elsewhere. It is usually treated with antibiotics.
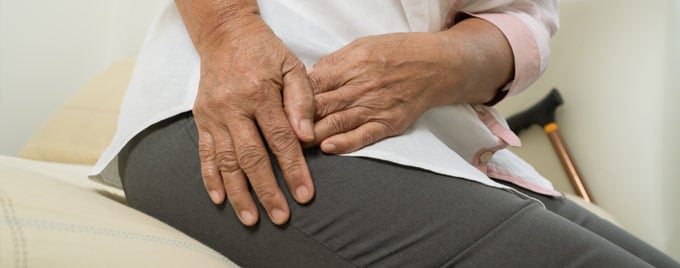
Causes of hip bursitis
Hip bursitis can affect anyone at any age although it is more common in women and if you are aged over 40 due to wear and tear of your hip joint over time. Being overweight also increases your risk as this puts extra strain on your hips.
Other risk factors for hip bursitis include:
- Bacterial infection of a bursa — this can occur if a bursa becomes damaged through trauma or if the skin or tissue around your hip joint becomes infected and the infection spreads to your bursa
- Bone spurs — bony growths often caused by osteoarthritis, which can irritate your bursae
- Conditions affecting your spine that consequently strain your hips — this includes:
- Arthritis eg ankylosing spondylitis, osteoarthritis, rheumatoid arthritis and gout
- Scoliosis
- Hip injury eg a fall or sudden, hard impact on your hip
- Overuse of your hip ie activities that involve repetitive movement of your hips or strain on your hips
- Your legs being different lengths — this can be present from birth or can develop during your childhood
Having a history of bursitis or past hip surgery also increases your risk of hip bursitis.
Hip bursitis diagnosis
If you’re concerned that you may have hip bursitis, see your GP. They will discuss your symptoms and ask how they affect your life. They will also perform a physical examination of your hip joint to check for any tenderness and assess its range of movement.
They may then recommend tests to help make a diagnosis. There isn’t one definitive hip bursitis test. However, there are several tests to help detect hip bursitis and rule out other conditions that cause hip pain, such as hip osteoarthritis, tendonitis, connective tissue injuries, snapping hip syndrome and conditions that affect your lower back.
Your GP may recommend any of the following tests:
- An X-ray — this can detect fractures and osteoarthritis
- Blood tests to check for inflammatory conditions eg ankylosing spondylitis and rheumatoid arthritis
- Bone scan — this can detect fractures or other bone damage that can’t easily be detected on an X-ray, as well as signs of infection or cancer
- MRI scan — this can detect fractures or other bone damage that can’t easily be detected on an X-ray, as well as early signs of arthritis and damage to your cartilage or tendons
- Ultrasound scan — this can detect excess fluid build-up caused by bursitis and torn tendons
Your doctor may also recommend removing the build-up of fluid (aspiration) in your affected bursa. This can help relieve the pressure on your hip joint and ease your pain. They may send a sample of the fluid collected to a lab to test for infection — this will determine whether you have septic hip bursitis.
Hip bursitis treatment
What types of doctors treat hip bursitis?
Hip bursitis treatment can be provided by several different types of doctor, depending on the underlying cause of your condition. You may be treated by your GP, a general medicine doctor, a doctor specialising in treating rheumatic diseases (rheumatologist) or a doctor specialising in treating muscles and bones (orthopaedic surgeon).
Non-surgical treatments for hip bursitis
Home therapies
There are several things you can do at home to treat your hip bursitis. Try to avoid activities that worsen your symptoms eg high-impact exercises such as running and jumping. Instead, try low-impact exercises such as swimming.
For temporary pain relief, you can apply ice packs to your hip for 10-20 minutes several times a day. Over-the-counter nonsteroidal anti-inflammatory drugs (eg aspirin, ibuprofen and naproxen) and topical anti-inflammatory gels and creams are also effective for reducing pain and inflammation. However, make sure you speak to your GP before using any NSAIDs as they are not recommended if you have certain health conditions or are on certain medications.
To reduce strain on your hip, you can try using a walking cane or crutch for a few days or a week. However, this is not a long-term solution as it is important that you continue to move around as much as possible to keep your hip muscles strong.
If you are overweight, losing excess weight will also reduce the strain on your hip to ease your hip bursitis symptoms.
Physiotherapy
If home therapies are not enough to relieve your hip bursitis, your GP may refer you to a physiotherapist. They can teach you specific exercises to stretch and strengthen your hip, which you can perform daily.
Steroid injections
Your doctor can give you a steroid injection, alongside an injection of local anaesthetic directly into the affected bursa in your hip. This treatment may provide relief from your symptoms for several months or in some cases, may permanently resolve your bursitis. If your symptoms return, you can have another steroid injection. However, it is not recommended to have more than two steroid injections as this can damage the tissues in your hip.
Aspiration
Aspiration involves using a needle and a syringe to drain the fluid in your affected bursa. This helps relieve the pressure on your hip and any pain. If your doctor suspects that you have septic hip bursitis, the fluid may be sent to a lab for testing to confirm this diagnosis.
Antibiotics
If you have septic hip bursitis, your doctor will prescribe a course of antibiotics to treat the infection and therefore prevent it from spreading elsewhere in your body. If septic hip bursitis is not treated and the infection spreads, it can become life-threatening.
Extracorporeal shock wave therapy (ESWT)
ESWT is a non-invasive procedure that involves applying low energy sound waves to your affected hip using a special device. These sound waves improve blood flow to your hip, which helps healing.
Needle tenotomy (percutaneous tenotomy)
If your hip bursitis is caused by damage to your tendons, your doctor may recommend needle tenotomy, which is performed under a local anaesthetic. This involves making tiny holes in your tendon using a needle. This encourages the growth of new, healthy tendon tissue.
Surgical treatments for hip bursitis
Surgery is not usually needed to treat hip bursitis. However, if non-surgical treatments for your hip bursitis are not effective, your doctor may recommend surgery. The type of surgery you have will depend on the underlying cause of your hip bursitis.
Bursectomy
This surgery involves removing the affected bursa in your hip. Over time, a new, healthy bursa will grow back and your hip will be able to function as normal.
A bursectomy can be performed using keyhole surgery, which uses small cuts and therefore has a faster recovery time than open surgery. A thin, telescope-like tube called an arthroscope is inserted into your hip via small cuts. Surgical tools are also inserted and used to cut out and remove the bursa. An arthroscopic bursectomy is an outpatient procedure, which means you won’t have to spend the night in hospital.
Tendon repair and iliotibial band release
Hip bursitis can be caused by iliotibial band syndrome. This occurs when the tendon that runs along the outside of your upper leg from your pelvis to your knee (the iliotibial band) becomes too tight or damaged through overuse. This causes increased friction when you move your leg and therefore irritates the trochanteric bursa in your hip. It can be treated through surgery to lengthen the tendon (iliotibial band release) or to repair it.
Osteotomy of the greater trochanter
This surgery involves cutting off a small part of the greater trochanter — the bony part of your hip where your thigh curves outwards. This can reduce any friction that is irritating the trochanteric bursa in your hip.
Hip bursitis recovery
Your recovery from hip bursitis will depend on the underlying cause and what type of treatment you receive. The recovery time, therefore, varies from several days to several weeks. If you have had surgery, you may need to use a cane or crutches for a few days and may have post-surgery pain for a few days, which you can manage with over-the-counter painkillers.
Hip bursitis prevention
You can reduce your risk of developing hip bursitis by avoiding activities that involve repetitive movement of your hips or that put it under strain. Performing exercises that help strengthen your hip muscles and retain their flexibility can also help — you can speak to your GP or a physiotherapist for advice on which exercises are appropriate.
If you are overweight, losing weight can help reduce the strain on your hips. If your legs are different lengths, you can be fitted with shoe inserts or have shoes specially made to compensate for the length difference.
Hip bursitis Q&A
What does bursitis in the hip feel like?
Hip bursitis can make your hip feel tender and painful. At first, your hip pain may feel intense and sharp and later become achy and dull. Pain may also radiate up your lower back and down your leg to your knee.
How do you get rid of bursitis in your hip?
Avoiding activities that worsen your symptoms, such as high-impact exercises (eg running and jumping) or exercises that extend your hip a lot (eg squatting), can help resolve your hip bursitis. Taking over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, applying topical anti-inflammatory creams or gels, and applying ice packs several times a day can also help. If these home therapies do not resolve your symptoms, see your GP. They may refer you to a physiotherapist, drain the fluid from your affected bursa and/or prescribe steroid injections.
How long does it take to heal hip bursitis?
Recovering from hip bursitis is usually quick, taking anywhere from a few days to a few weeks, depending on the underlying cause and the treatment you receive.
Is walking bad for hip bursitis?
Walking may worsen your hip pain and you may therefore need to use a walking cane or crutch for a few days or a week. However, it is important to stay as active as you can to keep your hip muscles strong. So if your symptoms do not improve after one to two weeks of avoiding high-impact exercises and taking over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs), see your GP.
Can sitting cause hip bursitis?
Hip bursitis is often caused by overuse ie activities that stretch and/or strain your hip joint eg running, jumping, cycling and squatting. However, once you have hip bursitis, sitting for prolonged periods of time can worsen your symptoms.
Does hip bursitis ever go away?
Yes, hip bursitis can go away after a few days or weeks by avoiding the activities that worsen it and taking over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs). If home therapies do not work, medical and surgical treatments are available. However, once you have had hip bursitis, you are at greater risk of developing it again.
Can massage help hip bursitis symptoms?
Massaging your hip may worsen your hip bursitis, particularly if you massage the tissue directly above your affected hip bursa. However, certain exercises can help — a physiotherapist can prescribe a programme of exercises to help your hip bursitis.
What exercise is best for hip bursitis?
Exercises that strengthen and gently stretch your hip muscles can help treat hip bursitis. A physiotherapist can put together an exercise programme for you. This may include exercises such as hip bridges, lying lateral leg raises and lying leg circles.
What foods should you avoid if you have bursitis?
Bursitis involves inflammation, so avoiding foods that promote inflammation may help. This includes processed meats (eg sausages, bacon, ham and smoked meat) as well as foods high in:
- Refined carbohydrates (carbohydrates where the fibre has been removed) eg bread, cakes, pasta, pastries, certain cereals and sweets
- Sugar or high-fructose corn syrup eg cakes, biscuits, pastries, sweets, fizzy drinks and certain cereals
- Trans fats eg margarine, fried foods and certain processed foods
How do you sleep comfortably with hip bursitis?
Avoid sleeping on the side of your body with the affected hip and try to sleep with a pillow between your knees to keep your hips aligned. You may also find that sleeping on a mattress with a foam topper helps by reducing the pressure on your hip.

