A cervical screening is a test offered to women between the ages of 25 and 64 as a way to prevent cervical cancer. It isn’t a test for cervical cancer itself, but checks for unhealthy changes to cells lining your cervix and for the presence of a virus called human papillomavirus (HPV).
What is HPV?
HPV refers to a very common group of viruses, which many people are infected with. The virus usually goes undetected without causing any problems or symptoms. Although there is no treatment for HPV, it’s usually resolved by your body in two years.
However, in some people, it can cause genital warts and abnormal cells that can sometimes develop into cancer.
The virus is easily contracted by skin to skin contact of the genitals and the sharing of sex toys. In regards to protection, although using a condom can help limit your risk of infection with HPV, it can’t offer full protection as there will still be some skin to skin contact in the genital area.
Girls and boys aged 12 to 13 can now receive the HPV vaccine. If you didn’t receive your vaccination at school, you may still be eligible up until your twenty-fifth birthday.
What is a cervical screening?
A cervical screening is the method used to detect precancerous and cancerous changes in your cervix as well as checking that your cervix is in good health.
Your cervix is the narrow opening from your vagina into your womb. The doctor or nurse performing the screening will collect a small sample of the cells lining your cervix to check if there are any changes in them.
Why is cervical screening important?
Cervical cancer is preventable. By making sure that you regularly attend your cervical screening, precancerous cells can be detected and removed before they develop into cancer.
This test saves 2,000 lives annually in the UK alone.
When to get a smear test
Women aged between 25-64 years should have a regular cervical screening, whether they are sexually active or not. For women aged 25-49 years, a cervical screening should be done every three years and for women aged 50-64 years, every five years.
The ideal time to have your smear test is one week after your last period. If you are not familiar with the dates of your menstrual cycle, you can monitor them beforehand so you have an idea of what date to make an appointment. However, if you can’t work this out, don’t let it deter you from booking your test. For two days before your test, it is advisable not to have sex, nor to douche or use spermicidal foams, creams or jellies as these can all obscure the detection of any abnormal cells.
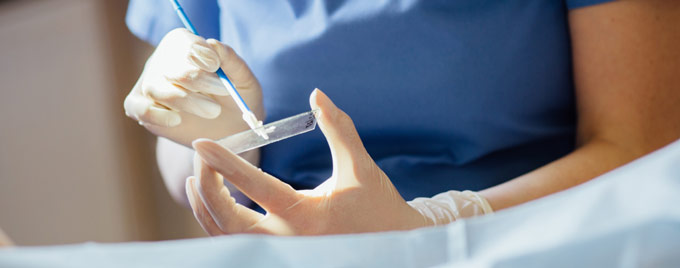
What happens at your smear test
On the day of your appointment, it’s best to wear comfortable clothes so you can undress easily.
The screening is usually performed by a female nurse or doctor and takes just a few minutes. You will be given privacy so you can undress from the waist down and will then be shown to an examination bed where you must lie on your back with a paper sheet to cover yourself.
There are five steps to the smear test:
- You will be asked to bend your legs, place your feet together and to allow your knees to fall open. Occasionally you may be asked to change position
- The nurse or doctor will then gently insert a lubricated plastic speculum into your vagina. A speculum looks like a long duck’s bill with a hollow centre. This can feel a little uncomfortable but if you relax, by slowly breathing in and out, this can help a great deal. You can practice breathing exercises before your appointment in preparation
- The nurse will carefully open the speculum to widen your vagina, so that they can see your cervix clearly. This part of the procedure can cause a few seconds of discomfort, but again breathing exercises can help relax you
- Using a soft, long, thin brush the nurse or doctor will take a small sample of cells from the neck of your cervix. This may cause a scraping sensation that will feel briefly uncomfortable
- Once the sample has been taken the nurse will close the speculum and gently remove it. The smear test will be complete and you can get dressed and leave
Occasionally light vaginal bleeding can be experienced for up to one day after the test.
Getting your results
The results of your cervical screening usually take up to two weeks by post. There are usually four possible results:
Negative result
No abnormal changes were found in the cells of your cervix and you tested negative for HPV. You will be invited to come for another regular cervical screening in three years (unless you are aged over 50, then it will be five years).
Unclear result
This result is recorded for a variety of reasons. Sometimes not enough cells were harvested during the screening. The results may have been unclear because you had your period or an infection. You will be asked to make an appointment to have the test re-done.
Mixed result
No abnormal changes were found in the cells of your cervix and you tested positive for HPV. You will be invited to have another cervical screening in one year.
Positive result
Abnormal changes were found in the cells of your cervix and you tested positive for HPV. This does not definitively mean that you have cancer but you will need further tests and/or treatment.
What to do if your results are abnormal
It can come as a shock if your cervical screening has shown the presence of some abnormal cells. But it is important to remember that this does not mean that you have cancer. Talk to your doctor or practice nurse if you are feeling anxious or worried. If you need to have further tests, you may feel stressed while waiting to have them.
The important point to remember is that the majority of women who are given further test results do not develop cervical cancer. If further tests confirm the presence of precancerous cells, you will have a colposcopy — a procedure that takes a closer look at your cervix and may involve a biopsy or treatment to remove precancerous cells.
Worried about your smear test?
Cervical screening is a very personal procedure that you may find stressful, embarrassing or intrusive. Some women find the whole idea such an ordeal that they decide against having the test. Although the procedure is quick and straightforward, you might feel uncomfortable about the idea of a stranger seeing such personal areas of your body.
Doctors and nurses are experienced in this procedure and will be on hand to help make you feel as comfortable as possible.
Often it is not knowing what is involved in cervical screening that can cause anxiety. Talk it through with your doctor, a family member or good friend, so that you know what to expect, or read about it from reputable websites online. If you have any questions, your doctor or nurse will be happy to answer them.
While most women would agree that having cervical screening is not the most pleasant experience in the world, consider that for a few moments of discomfort every few years, you gain the reassurance that you are considerably reducing your risk of ever developing cervical cancer.

