There are over two million people in the UK living with coronary artery disease, also known as ischaemic heart disease or coronary heart disease. It is a serious condition that causes the blood vessels supplying your heart (coronary arteries) to become narrowed or blocked due to atherosclerosis. Atherosclerosis is caused by the accumulation of cholesterol and other fats (atheroma) along the walls of your coronary arteries.
Who is at risk of coronary artery disease?
Although coronary artery disease can affect you at any age, it is more common as we get older, particularly in people with other health conditions, such as diabetes, high blood pressure, high cholesterol and/or a history of smoking. Being overweight or obese, or having a family history of the disease also increases your risk of developing coronary artery disease.
More men than women have coronary artery disease. However, women with coronary artery disease may have a higher risk of poorer outcomes after a sudden reduction in the blood flow to the heart, such as a heart attack. In fact, in women worldwide, coronary artery disease is the leading cause of death and in the UK, it causes twice as many deaths in women than breast cancer.
Coronary artery disease symptoms
The main symptom of coronary artery disease is chest pain, which is called angina and refers to chest pain caused by a reduction in the blood flow to the heart. The sensation of angina varies from one person to the next but is often described as a tightness across the chest or a feeling of pressure on the chest. This pain can sometimes radiate down your left arm and/or up to your jaw and often occurs after physical exertion.
When to see your GP
If you experience chest tightness when performing physical activities and this has been going on for several weeks or months, it is important to see your GP. Based on your symptoms and medical history, they may prescribe certain medications and/or refer you to a doctor specialising in treating the heart, a cardiologist.
If you’re experiencing sudden, unusual chest pain, pressure or tightness, seek urgent medical help at your nearest A&E. You may be having a heart attack.
Although some heart attacks occur after a sustained period of weeks or months of experiencing angina, most often, heart attacks occur out of the blue. This is often due to atherothrombosis ie when a blood clot (thrombus) suddenly forms next to part of your coronary artery that is narrowed by atheroma.
The clot causes the blood supply to part of your heart to be reduced or stop altogether, which causes chest pain or discomfort and is a heart attack. This can occur at any time, even when at rest. It is frequently mistaken for indigestion and is not always as severe as you may imagine it to be.
Getting a diagnosis for coronary artery disease
There are several different ways to diagnose coronary artery disease. Depending on your general health and particular risk factors, you will either have a non-invasive imaging test or an invasive coronary angiogram. The coronary angiogram remains the gold standard as it allows assessment of your coronary arteries, diagnosis of conditions affecting your coronary arteries and the option for treatment where appropriate by implanting a stent.
Coronary angiography
You will be awake during this procedure, while your doctor passes a thin, flexible tube (catheter) into a blood vessel via your groin or arm — the area will first be numbed using a local anaesthetic so you won't feel any pain.
Using dynamic X-ray imaging, the catheter will be guided through your blood vessels up into your coronary arteries, which supply your heart. A contrast dye will then be injected through the catheter. As this dye passes through your blood vessels, X-ray images (angiograms) will be taken allowing your doctor to see if any blood vessels are narrowed or blocked.
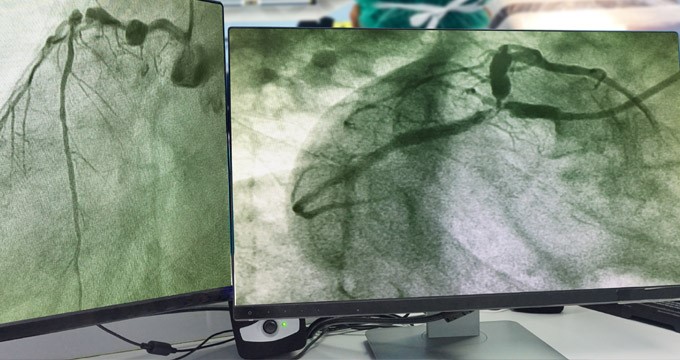
Treating coronary artery disease
There are multiple treatments for coronary artery disease, both surgical and non-surgical.
Medications for coronary artery disease
If you have received a diagnosis of coronary artery disease, your doctor will discuss medications that will help reduce your risk of having a heart attack. These include anti-platelet drugs that prevent blood clots (eg aspirin and clopidogrel) and statins that reduce cholesterol levels and independent of the cholesterol-lowering effect, will reduce the risk of heart attacks and stroke.
If you have angina, your doctor can also prescribe medication to help prevent or treat these episodes when they occur.
If you have already had a heart attack, you will be given medication to reduce your risk of further heart attacks, such as beta-blockers and angiotensin-converting enzyme inhibitors.
If medication alone is not effective at treating your coronary artery disease, your doctor will advise you about surgical treatments, namely a percutaneous coronary intervention (PCI) or a coronary artery bypass operation.
PCI
Your doctor will first perform a coronary angiogram to assess the extent to which your coronary arteries have narrowed. Based on what they find, they may decide to perform a PCI then and there, also known as a coronary angioplasty.
This involves inserting a tiny, deflated balloon into the narrowed coronary artery. Once in place, the balloon is inflated to widen the artery and then a metal scaffold called a stent is inserted and remains in place to maintain a healthy blood flow through the artery.
PCI is a minimally invasive keyhole procedure performed via insertion of a needle into an artery in your wrist or leg, through which devices needed to treat the narrowing of your coronary artery can be passed — all of this is done without you feeling anything. It is usually a day case, which means you can return home on the same day as your procedure. However, if your procedure is more complex and/or takes longer than expected, you may need to spend a night in hospital.
Coronary artery bypass surgery
If PCI is not appropriate, your doctor may recommend a coronary artery bypass. This involves grafting a vein or artery from another part of your body to your heart to bypass the need for the narrowed or blocked coronary artery. This will restore a healthy blood supply to your heart.
Whether you have a PCI or a coronary artery bypass will depend on your individual risk factors, other health conditions and which procedure will best suit your medical circumstances taking into account short, medium and long-term considerations.
Recovering from surgery
Recovering from PCI
As PCI is a minimally invasive keyhole procedure, the recovery time is much faster than with a coronary artery bypass. You may be able to return home on the same day as your procedure, and can usually return to driving after 48 hours and get back to all of your usual activities after a week.
You may need to have repeated PCIs in the future. However, if you take steps to reduce your risks, such as reducing high blood pressure, controlling diabetes and quitting smoking, the chances of needing further PCIs is considerably reduced and the stents themselves are engineered to last a long time.
Recovering from a coronary artery bypass
A coronary artery bypass is a major surgery with a six to eight week recovery time. As with any major surgery, there are greater risks than with a less invasive procedure. However, the results of a coronary artery bypass mean that you are less likely to need further procedures in the future and will have a durable treatment for coronary artery disease.
Life after a diagnosis of coronary artery disease
Whichever treatment for coronary artery disease you receive, making lifestyle changes to reduce your risk of the disease progressing is essential. This includes following a healthy, balanced diet, regular exercise, quitting smoking and taking any prescribed medication as instructed by your doctor.

