Glaucoma is one of the top three reasons why an adult in the UK ends up sitting in a hospital’s eye department. That’s unsurprising given glaucoma is one of the leading causes of blindness worldwide.
The damage glaucoma causes to your vision is irreversible, but thankfully due to excellent screening for the condition at opticians, less than 5% of the patients I initially see with glaucoma have suffered significant vision loss. This highlights why awareness and early detection of this condition is so important — it can help prevent debilitating vision loss from a disease that is often symptomless until it reaches advanced stages.
Preventing vision loss
Preventing vision loss from glaucoma starts by making sure you keep up with your regular eye tests at the opticians — these are free on the NHS if you are aged over 60 or aged over 40 and have a close relative with glaucoma.
The most common type of glaucoma that accounts for around 90% of cases, open-angle glaucoma, develops gradually over years. It’s painless and often without symptoms — that’s why open-angle glaucoma is often referred to as ‘the silent thief of sight’.
However, a simple check of your eye pressure at the opticians can detect whether you’re at high risk of developing glaucoma. This is because glaucoma is caused by raised pressure in your eye due to fluid building up inside it. This pressure damages your optic nerve, which transmits information that your eyes see to your brain.
Glaucoma can also be diagnosed at your opticians using a visual field test, where you press a button when you see a light shining in your peripheral (side) vision. Your peripheral vision is usually the first to be affected by glaucoma.
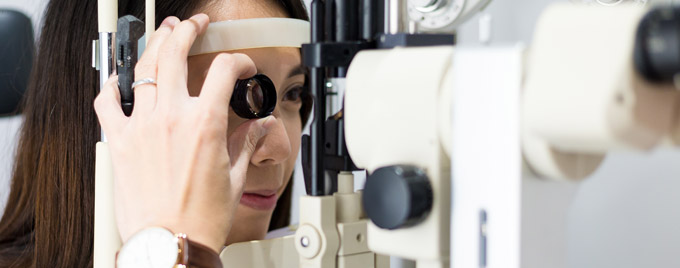
Advancing technology for diagnosis
Checking your eye pressure and visual fields are both quick, easy and well-established techniques for detecting glaucoma. But new technology means that today the chances of detecting glaucoma before your vision is affected are even higher. This is thanks to digital imaging, specifically optical coherence tomography (OCT).
OCT scanning is a quick, painless and non-invasive way to capture detailed digital images of the back of your eye (retina) and your optic nerve. This helps detect the earliest signs of damage by glaucoma or other eye diseases before you notice any changes in your vision.
Who’s at risk of glaucoma?
Glaucoma can affect anyone but you’re at a higher risk if you’re of Afro- Caribbean descent, a close relative has the condition and possibly if you have diabetes or are short-sighted.
Once detected, glaucoma treatments can help control your eye pressure and preserve your vision. Treatments are so effective that only 5-10% of people with glaucoma in the UK end up with advanced vision loss.
Without early detection and treatment, however, severe vision loss or blindness becomes much more likely.
Learning to live with glaucoma
Almost all the patients I see who’ve just received a diagnosis of glaucoma feel anxious and have concerns about their future. What will happen to their vision? Will they lose their driving license?
The reality is that most people with glaucoma who closely follow their treatment plan can continue with their everyday activities as usual at work and at home. As for driving licenses, only 12% of people with glaucoma in the UK lose their driving license, again thanks in large part to early detection, close monitoring and consistent treatment.
Once you have a diagnosis of glaucoma, it’s important to stick to your daily treatment regime even though your vision may appear normal — treatment is the only way to help your vision stay that way. This usually involves taking eye drops to reduce the pressure in your eye.
Depending on the type and severity of your glaucoma, you may need to apply eye drops to your affected eye(s) between two to five times a day. You’ll need to do this stringently every single day. This treatment is successful in 85% of cases.
Laser treatment and glaucoma surgery: who needs it?
Laser treatment for glaucoma includes selective laser trabeculoplasty (SLT). For most – but not all – people with glaucoma, it’s as effective as daily eye drops. It’s a low-risk, pain-free procedure that lasts for up to three years and is also offered as a first-line treatment alternative to drops.
Laser treatment is usually recommended if eye drops aren’t effective in reducing your eye pressure, or if for some reason, you’re unable to keep up with your treatment regime eg if you’re elderly and have stiff joints so struggle to apply eye drops.
If eye drops and laser treatment don’t work, glaucoma surgery called trabeculectomy may be recommended.
Whether or not you need to continue with daily eye drops after laser treatment or glaucoma surgery will depend on your individual case.
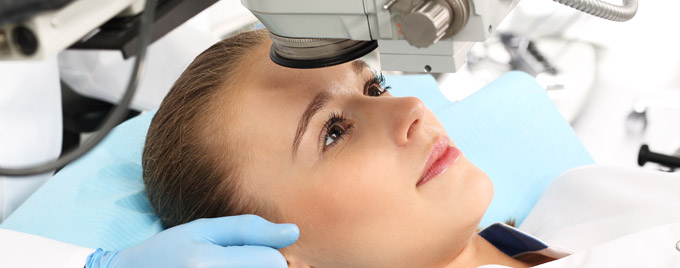
Glaucoma treatment: what’s changed?
Glaucoma treatments today are more effective than ever before. In the last 20 years, newer formulations of eye drops have been developed that work in different ways and are better at reducing eye pressure. What’s more, these formulations have now been combined, so rather than having to take several different kinds of eye drops, you can get 2-in-1 solutions. This makes it easier to stick to a treatment regime.
Most glaucoma eye drops are now also available in preservative-free formulations, which reduce side effects such as eye irritation, stinging and redness.
It isn’t just eye drops that have improved. Glaucoma surgery has advanced too. In the last five years, minimally invasive glaucoma surgery (MIGS) has revolutionised treatment. MIGS refers to a group of procedures that are either done by themselves or combined with cataract surgery. For glaucoma, it involves implanting a tiny stent or tube to drain excess fluid from the eye and therefore reduce eye pressure. This is a safer, faster and simpler surgery than a traditional trabeculectomy and appropriate for patients with mild to moderate glaucoma.
Glaucoma treatment: what’s next?
There’s an incredible amount of innovation in the field of glaucoma treatment, which will make it easier for people with glaucoma to manage their condition in the future. For example, instead of daily eye drops, sustained-release pellets are under development. This will involve injecting a pellet into the front of the eye, which will steadily release glaucoma medication every day for several months.
Researchers are also tackling glaucoma from a completely different perspective. Today the only thing we can change is eye pressure, bringing it down to prevent damage to the optic nerve. However, for a minority of people, this isn’t enough to prevent optic nerve damage. Research is currently underway to find out how to protect the cells of the optic nerve from damage.
Gene therapy is another big field that researchers are working on applying to glaucoma treatments.
Your glaucoma treatment
At Spire Healthcare, I and fellow consultants bring a wealth of experience and expertise in treating glaucoma and can offer a full range of diagnostic and therapeutic options. This includes OCT scanning, medications, laser treatment and glaucoma surgery.
What’s more, you won’t have to wait months to see a specialist, with easy access to appointments and your own dedicated consultant who you’ll see every time.
Author biography
Mr Venki Sundaram is a Consultant Ophthalmologist, specialising in glaucoma, cataract removal and macular degeneration at Spire Harpenden Hospital and at NHS Luton & Dunstable University Hospital. He is an Oxford graduate, who trained at the world-renowned Moorfields Eye Hospital in London, where he carried out high-level research into stem cell and gene therapy.
Visit Mr Sundaram's website: www.hertseyesurgeon.co.uk

