Ostetomies around the knee
28 February 2020
Mr Andrew Legg, Consultant Orthopaedic Consultant at Spire Methley Park Hospital, gives a brief explain as to what an osteotomy is, how it's performed and what to expect in the future.
What is an osteotomy?
A High Tibial Osteotomy (HTO) or Distal Femoral Osteotomy (DFO) is an operation that realigns the knee joint, to move where the body weight passes through the knee, from an arthritic part of the knee to the other side of the knee with normal articular cartilage.
Why would I want an osteotomy?
If you have varus (bow legs) or valgus (knock knees) and have pain on either the inside or outside of the knee, this may be due to this part of the knee being overloaded, failing, and ultimately developing arthritis. This is like the tracking being off on your car wheels; half the tyre wears out quicker than the other half. By moving where your body weight passes through the knee from the painful / arthritic compartment to the opposite compartment with normal articular cartilage, pain can be reduced without having a knee replacement and therefore preserving your knee; like your mechanic realigning the tracking on your car tyre.
Varus (bow legs): MRI image below on the right shows how the medial (inner) compartment is failing; the articular cartilage is becoming thin and therefore greater load is having to be taken by the subchondral bone which shows up white, causing pain.

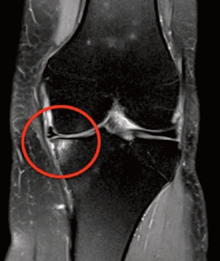
Why have an osteotomy rather than a total or unicompartmental knee replacement?
In young active patients wanting to preserve their knee joint rather than replace all or part of it with a knee replacement, an osteotomy is an excellent option to improve pain and function. Knee replacements can give reliable pain relief and improved quality of life, but can wear out or become loose over time, resulting in the need for revision surgery.
How do you perform an osteotomy?
Either the tibia (shin bone), femur (thigh bone) or occasionally both are carefully cut using a special saw after planning the correction using X-rays taken before surgery. After realigning the knee the bone is fixed with a strong plate and screws, which usually enables you to weight bear with crutches straight away.
The X-rays below show medial compartment arthritis. Planning X-rays before the HTO show the body weight passing though the medial (inner) arthritic compartment (yellow line). After the HTO the body weight passes through the lateral (outer) normal compartment (blue line).
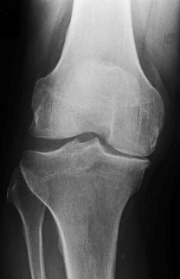
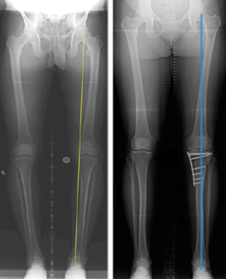
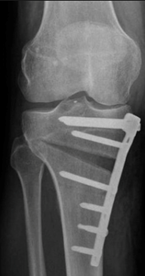
What is the recovery after an ostetomy?
You would stay overnight in hospital and usually be discharged the day after surgery. The plates used to stabilise the osteotomy are strong enough for you to weight bear straight away, but you will require crutches for 6 weeks. Physiotherapy is very important for you to regain you full range of motion and strength in your knee. By three months your function with day to day activities should be back to normal, but occasionally it can take a bit longer.
Will I need or can I have a knee replacement in the future?
Having an osteotomy does not prevent you having a knee replacement in the future although the plate and screws would knee to be removed beforehand. However, studies have shown that 70% of patients that have had an osteotomy at 10 years, and 60% at 15 years, have not undergone a knee replacement.
View Mr Legg's profile to book an appointment or to find out more.

