Macmillan Quality Environment Mark for Spire Thames Valley Hospital
29 September 2022
Spire Thames Valley Hospital is celebrating their achievement, after receiving a prestigious award that recognises high standards in cancer care.

We welcome your views on our website and invite you to take part in a brief survey when you've finished your visit.
Your response will help us improve the site and the experience we offer to visitors.
29 September 2022
Spire Thames Valley Hospital is celebrating their achievement, after receiving a prestigious award that recognises high standards in cancer care.

03 February 2020
Spire Thames Valley Hospital has maintained its ‘Good’ rating following an inspection by the Care Quality Commission (CQC).

20 January 2020
Cataracts are the world’s leading cause of blindness and surgery to remove them is the most regularly performed operation in the UK, with figures showing that around 300,000 procedures are carried out every year. Yet there are still thousands of people living in the shadows of cataracts.
20 September 2019
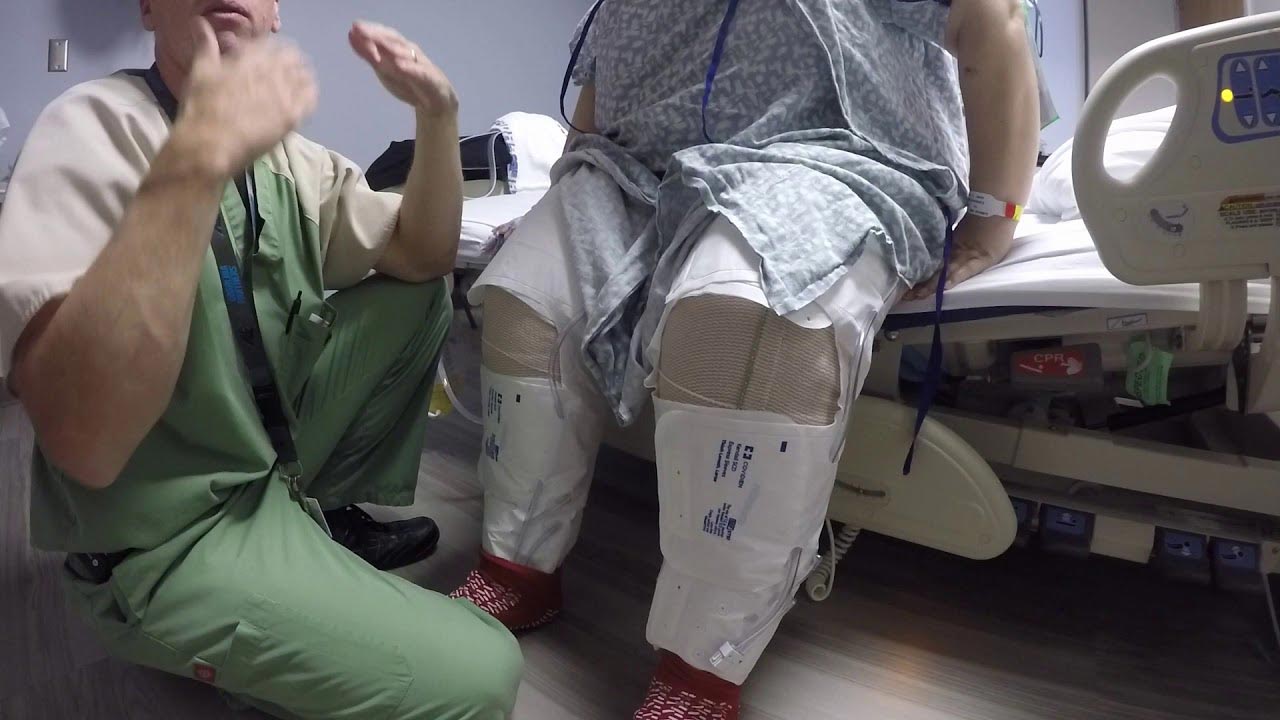
Spire Thames Valley Hospital have launched a campaign recently with a view to improving patients’ experience of surgery.

15 February 2019
Reduce recovery time with a double knee replacement.