Tell us what you think
We welcome your views on our website and invite you to take part in a brief survey when you've finished your visit.
Your response will help us improve the site and the experience we offer to visitors.
The interventional oncology service at Spire Southampton Hospital provides a range of treatments for primary and metastatic liver cancer (cancer that starts in another part of your body and then spreads to the liver).
The service is provided by a multi-disciplinary team of experts led by Dr Brian Stedman, consultant interventional oncologist, and is supported by consultant oncologists, consultant surgeons, consultant anaesthetists/intensivists and a nurse practitioner.
Treatments for cancer at Spire Southampton Hospital include surgery, chemotherapy, radiotherapy and interventional oncology. These pages provide information on interventional oncology techniques which are predominantly used to treat primary and metastatic liver cancer.
What is interventional oncology?
Interventional oncology uses minimally invasive techniques to deliver targeted treatment of cancer. Treatment is image-guided and is combined with some of the latest innovations in the treatment of cancerous tumours. These techniques minimise possible damage to other organs as a result of the treatment.
They are carried out by interventional oncologist Dr Brian Stedman who works alongside the rest of the interventional oncology team to determine the most suitable treatment for each patient.
View more information about chemosaturation at Spire Southampton Hospital.
List of our consultants
Chemosaturation (CHEMOSAT®)
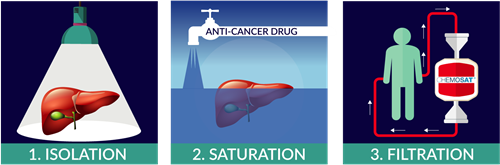
Chemosaturation therapy puts a high dose of an anti-cancer drug directly into the liver using minimally invasive techniques. During the procedure the blood supply to the liver is sealed off using two small balloons around the liver, helping to stop the anti-cancer drug spreading to other parts of the body. The blood is then filtered using the filter to remove most of the drug before returning it to the rest of the body. This allows for a strong local and thorough effect in the liver with limited whole body side effects.
Chemosaturation is used to treat primary liver cancer and metastatic liver cancer (cancer that starts in another part of your body and then spreads to the liver). It has proved to be effective in the treatment of ocular melanoma metastatic liver cancer.
As with any cancer therapy, treatment with chemosaturation therapy is associated with side effects. Please speak with your doctor for the full warnings and precautions associated with this procedure.
Southampton is currently the largest European centre providing chemosaturation treatment with extensive expertise in the management of ocular melanoma metastatic disease.
Selective Internal Radiation Therapy – SIRT
Selective Internal Radiation Therapy (SIRT) is also known as SIRTEX or Theraspheres Treatment. During the procedure very small radioactive beads are injected into the arteries that supply blood to the liver. The beads, which are smaller than the width of a human hair, are carried by the blood into the liver where the radiation treats the tumour cells.
SIRT is only suitable for patients who have malignant liver tumours (meaning that the tumour can invade and destroy nearby tissue and spread to other parts of the body). These tumours may have originated from the liver itself (hepatocellular carcinoma or HCC, cholangiocarcinoma, bile duct tumour) or have spread to the liver from elsewhere in the body (eg colon or breast cancer).
University Hospital Southampton, where the SIRT procedure is carried out, is one of ten UK centres selected to provide SIRT treatment under the current NHS commissioning through evaluation (CTE) process. For more information on CTE and the UK sites selected visit https://www.england.nhs.uk/2013/11/20/sirt-comm/
Transarterial Chemoembolisation – TACE
Transarterial Chemoembolisation (TACE) uses a small beads called microspheres that are filled with a chemotherapy drug. These are injected into the arteries that supply blood to the liver. Once in the liver they slow the blood and block off the blood supply to the tumour. The chemotherapy drug works over a period of around 14 days to treat the cancer cells.
TACE is used to treat cancer that has started in the liver.
Patient pathway
Your GP or oncologist will need to refer you to Dr Brian Stedman for one of the interventional oncology procedures. If you have up-to-date scans or imaging these will be reviewed by the appropriate multi-disciplinary team (MDT). If your imaging is not up to date you will need to have a dedicated liver MRI or a CT angiogram. These can be arranged for you through the interventional oncology office.
Once your scans are available, your case will be referred to the most appropriate MDT who will review your case and determine the most suitable course of treatment for you. This may be one of the interventional oncology procedures available or it may be for surgery, chemotherapy or radiotherapy treatment. The decision from the MDT will be communicated either through a clinical appointment, letter or telephone call depending on your circumstances.
Following your interventional oncology procedure you may be required to attend a number of follow-up appointments. These will be detailed to you following your discharge from hospital.
Patient stories
Brian Carney
West Yorkshire, England
“The optician said there could be something sinister. I didn't know what that meant but I knew it wasn't good.”
"It's not like a traditional chemotherapy programme where you're losing your hair and feeling nauseous for weeks and months at a time. With CHEMOSAT®, you have it, it's done, finished... move on."
Belinda Honeyman Lynch
"It has been much easier than I thought and the friendly faces at Spire Southampton we so reassuring and fantastic"
Interventional Oncology Patient
Spire Southampton Hospital
"I suffer from ocular melanoma, a rare condition that is considered terminal once it metastasises to the liver. Historically, there have been no effective treatments for managing tumour growth and life expectancy has been very limited. I presented with liver metastasis in September 2013 and, after having an immediate TACE (Trans Arterial Chemoembolisation) to buy me time to line up my first Delcath treatment, I had my first procedure in December 2013, followed by my second in January 2014. They were very effective in clearing the liver of the tumour burden, which allowed me to start off a course of Ipilimumab and, subsequently, Pembrolizumab. As all the new immuno drugs seem to be most effective when the tumour burden is low, Delcath was instrumental in not only addressing the immediate threat but in providing the drugs with an opportunity to provide a more enduring benefit.
Following a potentially suspect presentation in early 2015 I had two further procedures in April and July 2015, to prevent any progression.
For such a major procedure that offers such invaluable potential to prolong life, the Delcath procedure allows for a surprisingly fast recovery and an excellent quality of life between procedures. The first couple of days immediately following the procedure can involve some discomfort but it is very manageable and within a week you can expect to be back to living a normal life.
Finally I must say that, if you are considering having a Delcath procedure, you can do no better than choose Southampton Spire, for your care. The doctors and nursing staff are consistently outstanding. The surgeons, oncologists, interventional radiologists and the critical care consultants work seamlessly as a team to design a bespoke treatment plan to suit an individual patient’s condition. All hospitals seem to promise this approach but I have never seen it delivered anything like as effectively as by the team in Southampton. As with all complex procedures, experience counts and the team at Southampton have more experience of Delcath than anywhere else. The doctors are all experts in their field and they are also extremely approachable and patient in briefing patients on what they need to know, answering questions etc. The nursing staff and physiotherapists are exceptionally friendly, attentive and extremely professional. If and when I need any future Delcath procedures I wouldn’t consider having them anywhere else."

