Spire Clare Park Hospital invests in advanced robotic-assisted surgery
04 April 2025
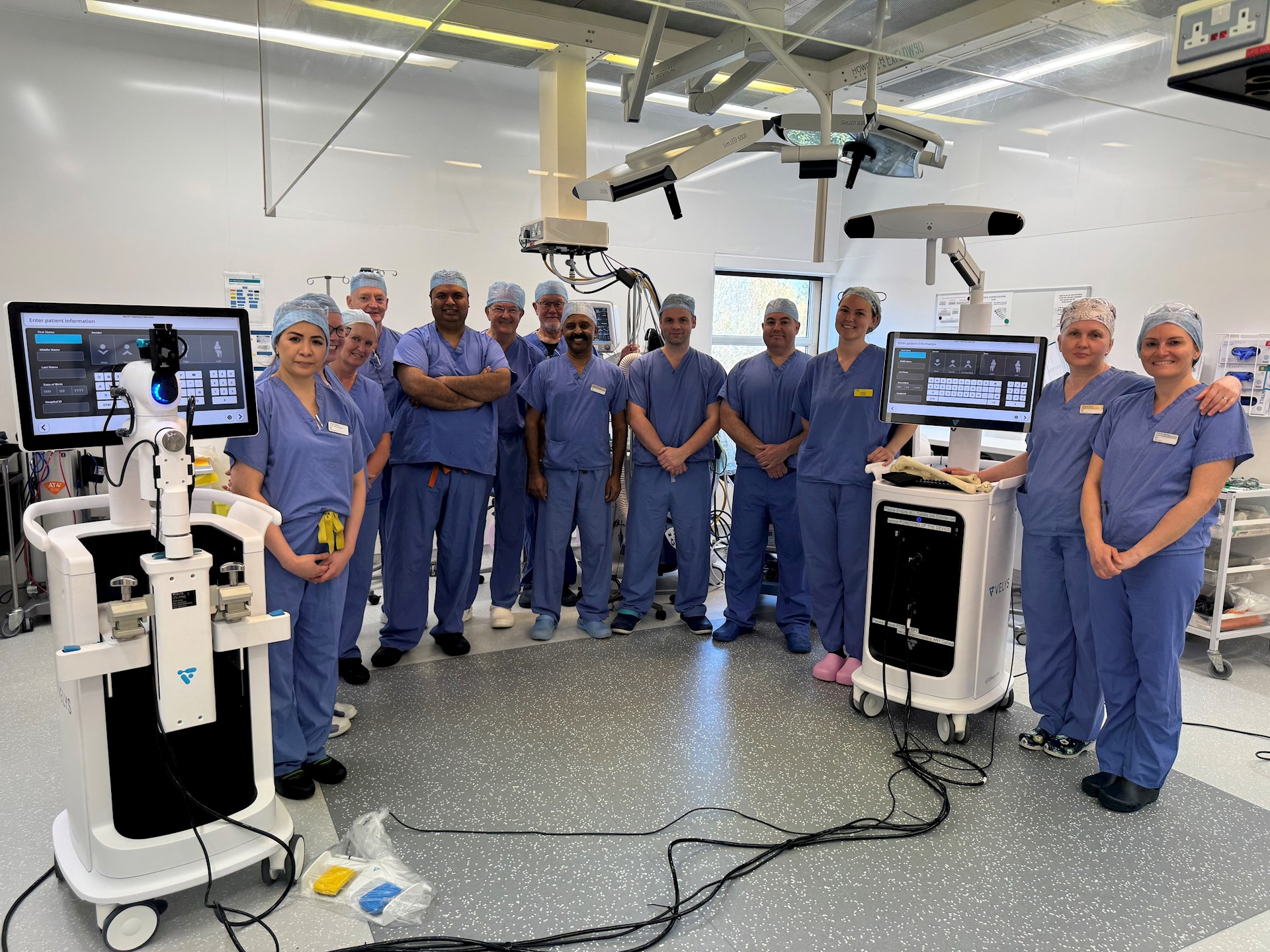
Spire Clare Park Hospital is proud to be the first hospital in the South of England to offer VELYS™ robotic-assisted surgery.
We welcome your views on our website and invite you to take part in a brief survey when you've finished your visit.
Your response will help us improve the site and the experience we offer to visitors.
04 April 2025
Spire Clare Park Hospital is proud to be the first hospital in the South of England to offer VELYS™ robotic-assisted surgery.

23 October 2024
Spire Clare Park Hospital has maintained its overall ‘Good’ rating, following an unannounced inspection of services by the Care Quality Commission (CQC) in March 2024. The previous inspection had been in 2022.

08 August 2024
Sam Creber, patient of Mr Seb Sturridge underwent a day case total hip replacement at Spire Clare Park hospital and “feel like me again now, the whole experience was life changing”.

17 November 2022
Spire Clare Park Hospital has maintained its ‘Good’ rating, following an unannounced inspection by the Care Quality Commission (CQC).

14 May 2020
Spire Clare Park Hospital sends around 50 healthcare workers to support the NHS in the response to COVID-19.
09 March 2020
Carpal Tunnel Syndrome, Trigger Finger and Dupuytren’s Contracture are three of the most common conditions to occur in the hand and can result in significant pain and dysfunction. Mr Gavin Brigstocke, Consultant Orthopaedic Hand Surgeon, discusses these conditions in more detail and the treatments that may be considered.
