The Heart of Care
29 February 2024
Our recent Dignity Day in February was a powerful reminder of this core value, an occasion for our hospital community to reflect on and celebrate the essence of dignified care.
We welcome your views on our website and invite you to take part in a brief survey when you've finished your visit.
Your response will help us improve the site and the experience we offer to visitors.
29 February 2024
Our recent Dignity Day in February was a powerful reminder of this core value, an occasion for our hospital community to reflect on and celebrate the essence of dignified care.
01 February 2023
New group of Paterson patients seen over 20 years ago to be contacted.
06 January 2022
Spire Parkway Hospital in Solihull has launched a major drive to become carbon neutral by 2030, with a package of environmental measures.
21 December 2021
Life took a downward spin for Philip Williams when hip pain put the brakes on his cycling passion.

25 November 2021
For over 14 years, Gemma Williams has dedicated her life to healthcare, but it was the onset of the Covid pandemic that really enabled her to find her true calling.

05 July 2021
Spire Parkway Hospital delighted to receive National Joint Registry Award.

14 January 2021
Derek tells of how failing eyesight almost put paid to his intricate painting skills as cataracts developed in both of his eyes.

04 March 2020
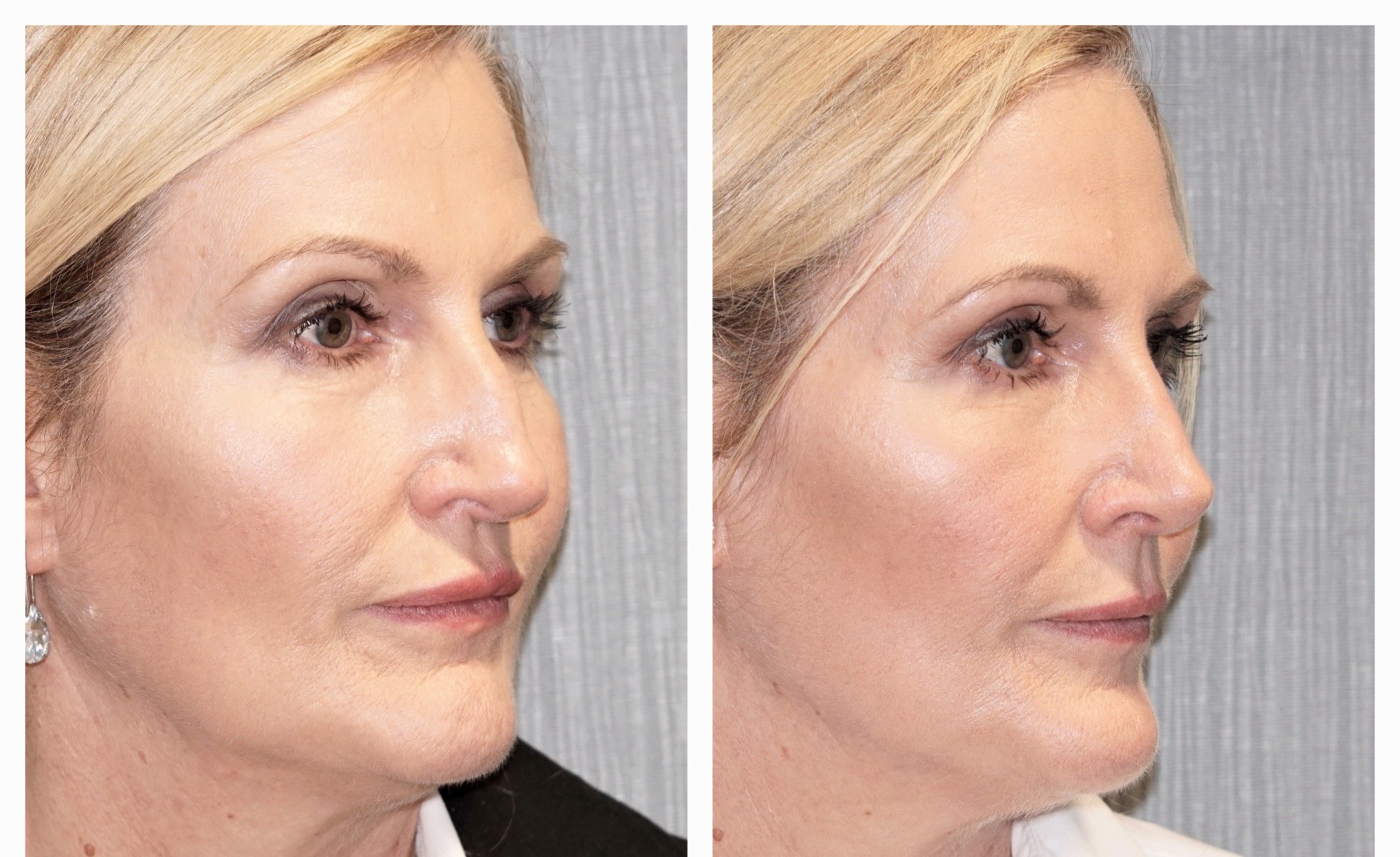
“I now finally have a nose that I actually like and I’m no longer embarrassed or concerned about having my photograph taken. It’s definitely given me the confidence I need to move forward." Read Helen's story of having a rhinoplasty at Spire Parkway Hospital.
12 December 2019
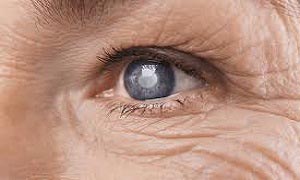
As his eyesight steadily deteriorated, 71-year-old Geoff Bell was worried that he might have to give up riding his beloved motorbike. But following two successful cataract operations Geoff is back on his Honda 750 and now doesn’t even need glasses when he’s out on the road.
09 December 2019
Spire Parkway Hospital has been upgraded to a ‘Good’ rating, following an inspection by the Care Quality Commission (CQC).
